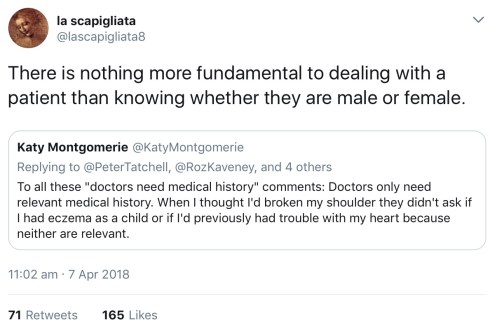
There’s been a lot of talk in the media recently about whether it is appropriate for doctors to ask patients whether they are trans. It is my opinion, from a medical perspective, that there’s nothing more fundamental to dealing with a patient than knowing whether they are male or female.
Transgender people can never change sex, but they can appear like the opposite sex. Not knowing this can jeopardise their medical care, and whenever they are seeing a doctor, he or she has duty of care to conduct appropriate history and examination in order to diagnose and treat them.
In the past, before the social contagion of transgenderism, advancements in plastic surgery and willingness to use puberty blockers and cross-sex hormones on gender non-conforming children, transsexual patients were both very rare and much more recognisable in context of their biological sex.
Now, a male looking teen presenting with abdominal pain could be pregnant. A broken arm could be a consequence of bone thinning due to puberty blockers which were given for gender dysphoria, instead of other causes which would be picked up without asking about trans status. Risk of complications such as blood clots, which often follow broken bones, would be increased in people who are or ever have been on certain hormones. Even medications which are routinely given to sick patients are known to interact with cross-sex hormones such as testosterone. And to come back to the male-looking teen who is biologically female and could be pregnant, well, that’s an extremely important piece of information if you are going to send that patient for diagnostic x-ray.
Being male or female makes certain diagnoses, complications, effects and side-effects of treatments, outcomes and prognoses more or less likely. Normal blood test values vary between the sexes and not knowing the true sex of the patient could lead to under treatment, over treatment, missing a diagnosis or making a wrong diagnosis.
Take the media reports of trans-women (biological males who are registered with their GP as “female”) receiving invitations for cervical screening even though they never had a cervix, while trans-men (biological females registered as “male”) are not receiving invitations for breast screening. Allowing ideology and religion to influence healthcare polices can lead to medical neglect and adverse outcomes for patients.
Transgenderism is a phenomenon closely associated with illness. Once we started to treat gender dysphoria, ambivalence and other psychological symptoms with medications and surgery, we have medicalised that person and given them an iatrogenic (treatment-caused) condition. Anyone with chronic medical condition knows they’ll be thoroughly quizzed about it every time they have new presenting complaint, or are seeing a new doctor. This is not discriminatory, it is best medical practice.
Trans activists can’t have it both ways – demand medicalisation AND doctors to ignore it, in order to accommodate their feelings. This would be edging closely to trying to control how professionals do their job, without having any knowledge or expertise in that job, or any responisbility for outcomes.
To many marginalised groups, certain questions by doctors can seem discriminatory of their social status, but there is a very good reason these questions are being asked. HIV status, Hep B and C are all common in certain populations, for example, but tattoos are more of a Hep C risk factor if obtained in prison than a tattoo parlour. Past history of somatic delusions and previous investigations that revealed nothing alters our approach to elusive somatic symptoms.
It’s impossible to do justice to explaining fully to a layperson just how intricately history, examination and treatment are connected in medicine, so I’ll just say that there is no medical presenting complaint I can think of where full history taking isn’t essential, and where knowing the sex of the patient, or if they are or ever were trans (and how far into transition they went ie. whether they took medications, which ones, for how long and whether they had surgery) would not be relevant.
Conflating biological sex with gender identity in a way that seeks to obliterate the difference between the two, or even make gender identity more important medically than realities of biological sex, is dangerous. This is why people who aren’t doctors can ask questions, but they cannot condemn medical process just because they don’t understand it.
ps.
Here’s an excellent article that futher explores how postmodernism infiltrated all areas of study, severely compromising evidence-based approach. I found it illuminating.
Only problem is she claims gender is not a social construct. Bullshit. Sex is not a social construct, it is a material condition, but any role someone is expected to play on account of their sex that has nothing to do with reproduction is by definition socially constructed and imposed. Gender says women are not supposed to work in building trades, for example. That would be hilarious to the women of many traditional cultures who *build their own damned houses*.
LikeLike